Unnatural changes in the cartilage and bones of the spine cause the development of the disease, which, in accordance with the ICD-10 code, refers to the localization of M42 and is called thoracic osteochondrosis. The middle part of the spinal column experiences less stress than the lumbar and cervical, but deformities are difficult to heal. The load is distributed unevenly due to the rounded configuration of the sternum, osteophytes and other dysplastic manifestations appear.
Symptoms and Signs
The disease occurs in the nucleus pulposus of the intervertebral disc, spreads to the fibrous fibrous ring and other parts of the vertebral segment, which ensure the mobility of the spine. Changes are manifested by compression, reflex or mixed neurological disorders and syndromes.
Pain manifests itself with physical exertion. There are different types of sensations:
- mild prolonged pain in the thoracic region is called dorsalgia;
- sharp and sharp colic, provoking a difficult inhalation or exhalation, leading to immobility of the muscles - dorsago.
Symptoms and treatment of osteochondrosis of the thoracic spine depend on the degree of wear and tear of the bone apparatus and the stage of aging, which are generalized and local.
Symptoms include:
- damage to the peripheral processes of the nerves (neuralgia), characterized by painful attacks along the intercostal vasoconstrictors;
- concentration of pain in the left side of the chest or the occurrence of a strong painful sensation of a surrounding nature;
- decreased mobility of the spine in the chest area;
- numbness in the arms and hands;
- decreased sexual function;
- the appearance of pain in the area of internal organs, can give to the heart, stomach, liver;
- lumbago in the neck, cheekbones and head, cough or a lump in the throat;
- arrhythmia, tachycardia, fever.
Signs of osteochondrosis are disguised as manifestations of related diseases, so the symptoms are ambiguous. Spinal nerves are concentrated around the spinal column; when they are clamped, signals are sent to different parts of the body and organs.
Causes of osteochondrosis
There is no exact information about what factors deform the intervertebral discs. A common reason for osteochondrosis is scoliosis or curvature of the spine, which is more often recorded in childhood and adolescence.
The theory considers such factors of vertebral deformity:
- dysontogenetic;
- hormonal;
- vascular;
- functional;
- involutive;
- infectious;
- immune;
- dysmetabolic;
- mechanical;
- hereditary.
The deterioration and aging of bones and cartilage occurs as a result of prior exposure to adverse conditions. Atrophic degenerations in the spine are predetermined by a genetic factor, and a disease with clinical symptoms arises under the influence of an exogenous and endogenous environment.
The consequence in the form of complications in the work of the vertebrae occurs when the process of destruction of complex substances prevails over their synthesis. An exacerbation occurs when the disk power supply is disturbed and there is a shortage of useful elements. The penetration of elements and dissimilation products decreases, cell viability decreases, and parts of cells accumulate due to self-destruction. The production of complex proteins is reduced, collagen fibers are destroyed.
The mechanical effect on the annular connective formation increases, the layered structure is disorganized, the fibrous skeleton is torn. The disc is bruised under the influence of biomechanical factors and body movements, and its fixation ability decreases. Blood vessels and nerves can grow into the annulus due to a decrease in hydrostatic pressure.
Diagnostic methods
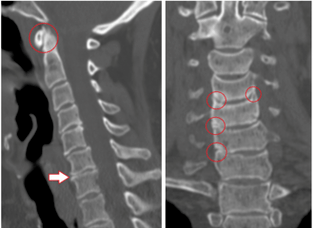
In the process of recognition, radicular, pain, reflex, myotonic, autonomic and vascular factors are identified. The best method of examination is difficult to identify, because in each case, the diagnosis is made individually.
The main methods are:
- X-ray diagnostics;
- CT scan;
- Magnetic resonance imaging.
X-ray analyzes the condition of the spine, images are given in oblique, lateral and direct projections. Sometimes, for a photo, a person bends, unbends, or bends to the side.
Contrast radiography is divided into the following studies:
- pneumomyelography - 20 to 40 ml of air is injected into the spinal canal;
- angiography - 10 ml of contrast agent is injected into the vertebral lumen and 7 to 9 images are taken in 2 - 3 seconds;
- myelography - an injection of a coloring liquid is made into the subarachnoid lumen, followed by a transillumination of the structure;
- discography - the stained substance is injected directly into the disc for localized examination.
Computed tomography evaluates the bone and tissue structure, the state of blood vessels. The painless method takes three-dimensional images in a few minutes.
Benefits of CT:
- high detection speed;
- screening of "dumb" areas during diagnostics in motion;
- the possibility of multispiral angiography;
- recognition of long objects with obtaining high-quality low-thickness cuts.
MRI uses a machine's magnetic field, which builds hydrogen atoms in the human body in parallel with the action. The particles signal, the response is recorded. The tomograph recognizes the waves and shows the result on the screen. There is no radiation with MRI, the method is less dangerous, but not recommended for pregnant women.
Treatment and prevention
It is necessary to treat osteochondrosis in several stages, the complexity depends on the severity of the disease, contraindications and body resources.
Methods:
- drugs and medication;
- methods of physiotherapy, exercises for removing clamps, relieving the patient's condition;
- operation.
There is a direction of kinesitherapy, within which it is possible to cure problems of the spine in the form of a hernia, spondylosis with rehabilitation gymnastics. Also, a method of recovery after surgery has been developed.
Yoga exercises help adult men, women, a child to overcome pain, warning that the main thing is a psychological attitude.
Medicines
Medications are prescribed by a neurosurgeon or neuropathologist in accordance with the card and medical history. Patients take medications in a hospital or at home, the main thing is to follow the instructions and not deviate from the intake regimen.
Common medicines:
- NSAIDs relieve pain, fever and inflammation;
- muscle relaxants lower the muscle tone of the skeletal skeleton;
- hormones reduce neuralgic pain;
- vitamins B2, B6, B12, A and C are taken during remission and for simple prophylaxis;
- diuretics relieve swelling and release pinched radicular nerves;
- neurometabolic stimulants improve the metabolism in nerve tissues;
- chondroprotectors restore the cartilage of the vertebrae after damage.
Sometimes the patient does without medication at the first stage of the onset of unpleasant sensations. It is enough to exercise, use a massager.
Physiotherapy

This type of exposure is used in conjunction with drug treatment or separately. In addition, bed rest is applied, heat is applied to the affected area. Folk recipes are used to relieve pain.
Physiotherapy in a medical institution includes procedures:
- ultrasound and phonophoresis;
- shock wave therapy;
- detensor impact;
- laser therapy;
- electrotherapy;
- magnetic waves;
- mud therapy and balneotherapy;
- massage.
Ultrasound involves the effect of high-frequency waves on tissues, which reduces pain sensitivity. With ultraphonophoresis, pain relievers and anti-inflammatory drugs are added for their better delivery to the affected areas.
Shockwave therapy is the transmission of an acoustic wave to the painful area, it is used to improve blood circulation, speed up metabolism. Detensor therapy consists of stretching the spinal column using the patient's body weight.

Laser therapy is based on the helium-neon generation of lasers to activate bioelectric currents in nerve fibers. The laser acts on inflamed nerve roots in the paravertebral region along the thoracic region.
Electrotherapy improves nutrition and metabolism of products in tissues, and impulse currents affect nerve sensory endings. Low frequency waves relieve acute pain and are used as an initial aid.
Magnetic therapy is used to relieve swelling, spasms, and inflammation. A magnetic wave inductor is placed on the affected thoracic region. Balneotherapy and mud therapy consists of swimming in pools, taking baths, contrast showers for treatment and during recovery. Metabolism is normalized, blood flow to the affected areas is accelerated, pain and inflammation are reduced.
Therapeutic massage for osteochondrosis of the thoracic spine is vacuum, point and lymphatic drainage, improves blood microcirculation, tissue nutrition, and tones the muscles. The sessions are conducted by a competent specialist, if you trust the spine to amateurs, dangerous consequences can ensue. Massage is prescribed after the end of the acute stage, the first session should not exceed 10 minutes.
Operative treatment
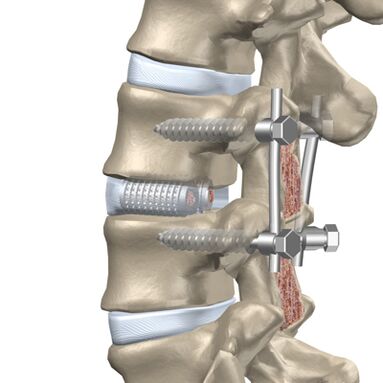
The patient is indicated for an operation if medical treatment, massage and other procedures do not alleviate the condition.
The intervention is divided into 2 stages:
- elimination of the cause of severe pain (decompensation);
- stabilization of the spinal column.
By means of the posterior approach, a facetomy is performed, becausefacet joints can press on nerves. Foraminotomy is the expansion of the radicular canal through which the nerve leaves the vertebra. Laminectomy removes the posterior portion of the vertebra, which protects the spinal lumen and presses on the brain due to deformity. Laminotomy involves enlarging the canal opening, where the spinal cord is located, while removing a separate fragment of the posterior region of the vertebra.
Anterior surgery is performed if there is a protrusion (bulging of the vertebral disc towards the spinal lumen) or a hernia protrudes towards the canal.
The following methods are used for front decompression:
- discectomy - removal of an entire disc or a separate part of it;
- corpectomy - removal of an entire vertebra and adjacent disc followed by implantation.
Discectomy and corpectomy lead to column destabilization and increase the risk of neurological defects. Rigid fixation or fusion of three vertebrae (fusion) is used.
Prevention of chest osteochondrosis

Exacerbations of the disease reduce the ability to work and the quality of human life, therefore, special attention is paid to prevention. As a result, vertebral degeneration appears later and disability is avoided.
Methods for preventing the disease:
- decrease in physical activity on the spinal column;
- you cannot stand still for a long time without changing the supporting limb, you can lean on an improvised object or a wall;
- it is not recommended to sit at a desk for a long time and when working with a computer, you need to take active breaks, walk around;
- mattresses and orthopedic head restraints are selected for sleeping;
- while running and walking, you need to avoid sudden sudden turns and jumps, walk in shock-absorbing shoes with small heels;
- carry weights no more than 10 kg, lift gradually from a sitting position.
In the car, you need to use bolsters for the back and head restraints, while the driver's seat must be rigid. Work cannot be performed in a half-tilt position, you can stand or sit. Well-developed muscles support the skeleton, so they pay attention to feasible physical education and hardening.
Possible complications
The disease develops for a long time, sometimes pain symptoms do not come immediately. Any degenerative changes in the thoracic region lead to the appearance of pathologies.
Types of complications:
- pathology of the heart vessels with subsequent myocardial infarction or angina pectoris;
- intercostal neuralgia or inflammation of the peripheral nerves with chest pain from root compression;
- protrusion of intervertebral discs.
Complications occur with advanced forms of osteochondrosis, so timely treatment in the early stages will help to avoid concomitant diseases.

























